By Rafael Lozano
Guest columnist
In an epidemic, public communication is not an accessory: it is part of outbreak control. And it should not act with grandiloquence or as propaganda, but as a device of trust that does three things at once: tell the full truth without stridency, translate risk into concrete behavior, and protect social cohesion without asking reality to stay silent. Data with context, urgency without panic, and a message always grounded in “what should I do today.”
That standard implies a rule of communication. In 2026, information is not “contained”; it is framed. If authorities try to manage data to avoid a headline, the message ceases to be health-related and becomes political (“they’re hiding it,” “they’re sugarcoating it”). And then the outbreak gains an advantage that is not biological but social: distrust, rumor, resistance, fatigue. Transparency is not a moral gesture; it is a control measure. This is part of the contemporary ABC of risk communication: speak early and often, honestly, even amid uncertainty, and with a single, coordinated voice.
Here, it is worth recalling recent memory. One negative aspect of the Covid pandemic was precisely communication. Even with centralization, it was riddled with contradictions, technical jargon that did not guide behavior, shifts in criteria without sufficient explanation, and a recurring impulse to assign blame.
Moreover, there was a particularly harmful shortcut: moralizing risk. “The obese,” “the diabetics” appeared as a convenient explanation, almost as if they were to blame for getting sick and for overwhelming services. That language was not only unjust: it was counterproductive. It stigmatized those who most needed guidance and care, reinforced the idea that illness is a personal failure rather than a constructed vulnerability, and weakened trust in the system. An epidemic is not controlled by blaming: it is controlled by reducing exposure, facilitating access, and communicating without humiliating. That red line must not be crossed again.

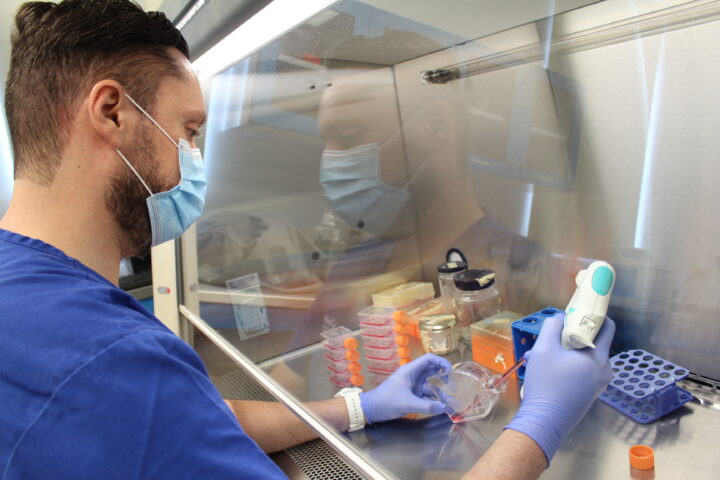
That said, it is worth acknowledging what is working in the measles epidemic. At the federal level, a relatively sober framework has been maintained: speaking of large figures (millions of doses, massive deployments) without inflaming public sentiment, insisting on the correct axis—vaccination and completing schedules—and pairing it with logistics: where, when, who is due, how hours are extended, how deployment is organized across territory. That combination reduces anxiety because it turns an abstract phenomenon (“there is an outbreak”) into a concrete route (“check your schedule, locate your clinic, go today”). In crises, many campaigns fail not because of a lack of vaccines but because they fail to translate the message into action.
Precisely for that reason, two recent episodes stand out as missteps, not because they negate the positive, but because they contaminate it. They are mistakes that cost double: they damage credibility and shift public conversation toward what is least helpful.
The first occurred where it should not have: at a press conference. Political authority intervenes when there is a possibility of reporting territorial differences, arguing, “Let’s not stigmatize.” The stated intention may sound reasonable, but the public signal is the worst: “don’t say that.” In a space designed for accountability, any gesture of restraint is read as data control, and controlling data does not avoid headlines—it worsens them. If one wants to avoid stigma, the modern solution is not to silence the map: it is to explain it with context and action.
The second misstep, however, is more serious and revealing. A federal authority presents gaps in seroprevalence (immunity) by age/cohort. It ties them to six-year political terms and to the names of former presidents as an explanation for the lag. Here, the problem is not health history; it is the emergency framing. In the midst of an epidemic, that maneuver shifts the focus from “what do we do today” to “who was to blame,” and activates what a crisis does not need: politicization, rebuttal, counter-rebuttal, wear and tear. The cost is not only discursive: it is operational, because every media minute consumed by the quarrel is a minute lost for the behaviors that cut transmission: getting vaccinated, completing schedules, seeking care without spreading contagion.
Moreover, that framing has a collateral effect: it turns a technical targeting tool—identifying cohorts with gaps—into partisan ammunition. If you give a politician graphs labeled with presidents, you are not giving epidemiology; you are giving labels. The result is predictable: the simple, actionable narrative (“young adults with incomplete schedules: come today, here”) is lost, and the quarrel takes over. In epidemics, the past serves for the report; spokespersonship, by contrast, must be operational.
In both cases, the same failure is repeated: reputation before cooperation. In one, data are covered up; in the other, data are labeled. When spokespersonship is shield or ammunition, it is no longer public health. In epidemics, communicating is intervening. If cooperation is not produced, the outbreak is fed. These errors are not managed: they are corrected the next day and prohibited the following week. If they are tolerated, they become the norm.
References for further reading
- CDC — Crisis and Emergency Risk Communication (CERC):
https://www.cdc.gov/cerc/media/pdfs/CERC_Introduction.pdf
- PAHO/WHO — Risk and Outbreak Communication
https://www.paho.org/en/topics/risk-and-outbreak-communication
Author
Rafael Lozano is a Full Professor in the Department of Public Health at the Faculty of Medicine of the National Autonomous University of Mexico (UNAM) and Professor Emeritus in the Department of Health Metrics Sciences at the University of Washington. rlozano@facmed.unam.mx; rlozano@uw.edu
The opinions expressed in this article do not represent the position of the institutions where the author works.